Joint Health Basics: Understanding Arthritis Symptoms

Arthritis is a group of joint disorders that cause mild to severe inflammation, stiffness and pain. In general, arthritis affects older adults, and some forms are simply a natural part of the aging process. Arthritis symptoms are seen in nearly a quarter of elderly Americans, with more than 50 million people affected. The condition can limit your range of motion and cause pain that’s mild or severe. Arthritis symptoms tend to be more pronounced among older adults due to the natural aging process.
There are over 100 types of arthritis that occur due to a variety of reasons. Some result from underlying conditions like autoimmune diseases, infections or viruses, while others happen due to injury or increasing age. Depending on the cause, arthritis can also be a lifelong condition that has no cure. In some cases, however, certain types of arthritis are treatable or can even resolve themselves.
Arthritis is one of the most widespread chronic conditions in the world. The most common types of arthritis include osteoarthritis, rheumatoid arthritis, gout, ankylosing spondylitis, psoriatic arthritis and juvenile arthritis. Moreover, some arthritis types run in the family, so there’s a possibility that you may develop the types of arthritis that your parents or immediate family members experienced.
Symptoms of Arthritis
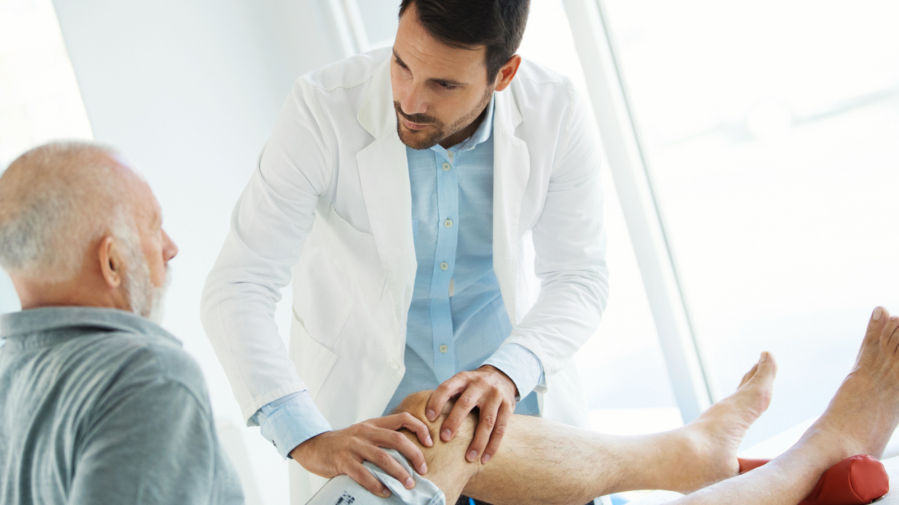
The symptoms you experience will vary based on what’s causing your arthritis. Some symptoms may occur suddenly, while others come on gradually and grow more severe over time. Common symptoms of arthritis include:
- Swelling
- Joint pain
- Limited joint movement
- Stiffness
- Redness
- Extreme tenderness
- Warmth over the joint
Arthritis can affect large joints and small joints. Commonly affected joints include the:
- Back
- Neck
- Knees
- Shoulders
- Fingers
- Wrists
- Toes
- Elbows
- Arms
Signs will also vary based on factors that include your:
- Age
- Weight
- Gender
- Diet
- Lifestyle
It’s usual for people with some form of arthritis to develop a low-grade fever during a flare-up period when symptoms are stronger, especially if the condition is related to autoimmune causes. If your fever persists or your fever spikes, you should see a doctor as soon as possible because you may be experiencing an underlying infection.
It’s essential to see a doctor if you experience symptoms of arthritis — you need a definitive answer about what’s causing your condition. While the cause might simply be related to aging, you’ll also want your doctor to double-check to determine whether other causes are possible. Other conditions can produce symptoms that are similar to arthritis. Knowing what’s causing your symptoms can help your doctor develop an effective treatment plan. Conditions that can produce symptoms that mirror arthritis include:
- Osteoporosis
- Hypertrophic osteoarthropathy
- Multiple myeloma
- Osteoporosis
Specific activities may cause your symptoms to improve or worsen. You may notice that your pain improves when you stretch and exercise, or you may find that your pain worsens when you do certain activities. For example, typing is a repetitive activity that can cause arthritis symptoms to feel more severe.
Specific forms of arthritis can cause additional symptoms not mentioned above. Lupus and rheumatoid arthritis can cause you to develop fevers and issues related to organ functioning. If you start to develop fevers, sudden and severe pain, or any issues related to your organs, visit a doctor immediately; you could have a painful underlying condition. You may experience edema, which is a sign of poor circulation, or diarrhea, which is a problem related to your small intestine.
Severe arthritis can cause organ failure. If you notice any unusual symptoms, experience nausea or have difficulty breathing, see a doctor as soon as possible.
Causes of Arthritis
In general, a breakdown of the cartilage in your joints is responsible for causing arthritis. The most common form of arthritis is osteoarthritis, which mostly occurs due to older age. Cartilage separates your bones and joints to make moving them a smoother, easier process. During routine activities, your bones experience pressure. Cartilage protects your bones from the wear and tear that this pressure causes. Over time, this cartilage becomes damaged or wears down. This process can occur gradually when arthritis results from aging and can occur suddenly if arthritis develops due to disease, a virus or another condition.
The causes and risk factors of other arthritis forms depend on the type of arthritis you have. Certain types of arthritis, such as those caused by autoimmune conditions, can be genetic. It’s important to know if arthritis runs in your family and to provide this information to your doctor.
Rheumatoid arthritis is a type that occurs because your immune system attacks your body’s joint lining and cartilage. The reason for this condition is unknown, and it can affect both children and adults. The most commonly affected joints include the fingers, knees, wrists, toes and elbows. Within a few years, these body parts can degenerate and change shape, becoming more difficult to use.
Ankylosing spondylitis is a type of arthritis that affects your spine and pelvis. Eventually, this type of arthritis can cause your spinal cord to fuse. Ankylosing spondylitis arthritis is also an autoimmune condition. The symptoms of this condition are most prevalent among adults assigned male at birth and will start to develop before age 30. The disease is systemic, meaning that it affects your entire body. It’s unknown what causes ankylosing spondylitis, but the condition can produce painful and uncomfortable symptoms.
Other conditions can also cause symptoms that are similar to arthritis. These conditions include osteoporosis, which causes your bones to lose density and become brittle, and multiple myeloma.
Repetitive motions can also cause arthritis to develop. Many athletes, dancers and people who work in industries that involve manual labor are likely to develop arthritis. Some people can even develop arthritis from typing for extended periods. People who place stress on their joints, cartilage and ligaments are at risk. If you’re an athlete, you may develop arthritis from your routine or as a result of an injury. You may notice that certain repetitive motions are causing an aching sensation in your joints. In that case, see your doctor promptly so they can evaluate your symptoms.
People who are overweight have a higher risk of developing arthritis because excess weight places stress on the bones. If you’re overweight, your arthritis can become more severe, and it can worsen quickly. Losing weight may help to slow down the progression of your symptoms.
Diagnosing Arthritis

To diagnose arthritis, your doctor will conduct a physical examination and ask questions about your personal and family medical histories. X-rays can show damage from osteoarthritis. Blood and urine tests can assess any potential damage to your organs and other bodily systems. A rheumatologist is a specialist who treats arthritis and related conditions, and you may begin working with one of these professionals after your diagnosis so you can receive specialized treatment.
Health History
Your doctor will begin by asking you routine questions related to your personal and family health history. For many types of arthritis and arthritis-related problems, symptoms run in the family. You can better understand your conditions and symptoms based on your family’s experiences and medical records.
Your family’s medical history can also help predict whether you’ll develop arthritis and at what age. And, both your personal and family health history can also reveal whether you’re at risk for certain conditions that cause arthritis. You may not have started experiencing symptoms, but your doctor will want to screen you as a precautionary measure. Based on your answers, the doctor might choose to conduct tests or refer you to a rheumatologist, a physician specializing in diagnosing and treating arthritis and related disorders.
Physical Exams
A doctor will conduct a physical exam to test your range of motion and flexibility. These tests are part of routine physical exams, so your doctor can track any changes over time. They typically check how well you can rotate your joints. If you have arthritis, you may notice that it’s painful when the doctor turns your joints. By feeling your joints, the doctor can check to see whether any fluid is accumulating in them. A physical exam will also help your doctor determine whether you’re experiencing arthritis or you’re experiencing symptoms similar to another condition that may or may not be closely related.
Testing
Blood tests can reveal whether or not you have an underlying infection and can also check for certain autoimmune conditions and organ damage. Generally, blood tests are part of a routine physical exam. Doctors may order specialized blood tests when they suspect arthritis or a family history of the condition.
A doctor may need to extract joint fluid to confirm arthritis and to determine the cause of your pain. After removing the joint fluid, a lab technician will examine the sample under a microscope to complete a detailed analysis. The sample may reveal crystals or other indicators that can help definitively diagnose the cause of your arthritis.
X-rays
X-rays can show whether conditions such as osteoarthritis, chronic gout and rheumatoid arthritis have damaged your bones and joints or caused deformities. In general, severe joint damage doesn’t occur until arthritis reaches its later stages. In any case, some people may not have noticed that they’ve been living with arthritis.
X-rays can also show whether certain bones are broken or have been broken in the past. These types of injuries, even when healed, can mimic symptoms of arthritis. An injury can also cause arthritis to develop in that particular part of your body.
Early on, especially with rheumatoid arthritis, X-rays do not show damage. Instead, the X-ray can show swelling and diminished joint space. Once the condition advances, the bones will begin to degenerate. Regular X-rays and imaging tests may be necessary to check the progression of the disease.
Treatments for Arthritis

The treatment you receive for arthritis will vary based on the type of arthritis you’re diagnosed with. Physical therapy can effectively treat some forms of arthritis. Other treatments include medications, anti-inflammatory drugs, herbal supplements, support splints, immunosuppressant drugs, paraffin wax drips, hot packs, cold packs and surgery.
There is no cure for arthritis. Treatments will alleviate symptoms; slow down the progression of the disease; or treat the underlying disease, disorder or condition. In some cases, there’s also no cure for the situation or condition that’s causing arthritis.
Your doctor will prescribe treatment based on the causes and symptoms of your specific case. Common treatments include exercise, lifestyle changes, support braces and dietary supplements.
- Physical Therapy: Your doctor may prescribe you a physical therapy regimen so you can learn exercises and routines that may help alleviate pain and other symptoms — or even the progression of your arthritis — in the long run.
- Medication: Over-the-counter painkillers may alleviate symptoms. Prescription drugs are available to relieve pain and suppress your immune system. Other drugs block the production of enzymes that cause inflammation. Some anti-rheumatic and immunosuppressant drugs can help alleviate arthritis that’s caused by an autoimmune disorder.
- Surgery: Many people with severe arthritis require joint replacement surgeries. With these procedures, the surgeon will rebuild the joint with a prosthetic. A surgeon may also choose to replace the natural joint fluid with synthetic joint fluid.
- Exercise: Regular, low-impact exercise can help prevent arthritis. If you’re moving and stretching, you’re less likely to feel stiff. In any case, most types of arthritis are impossible to control, primarily if they’re related to an autoimmune condition, disease or injury. Maintaining a regular exercise routine can help prevent arthritis from developing. Stretching improves flexibility, which can also minimize arthritis pain and stiffness.
- Diet Changes: A diet that’s high in calcium can help alleviate arthritis symptoms. You also might choose to take calcium supplements, with your doctor’s guidance. Some research has shown that antioxidants such as vitamin C can help slow down the effects of osteoarthritis. Fruits rich in folic acid can alleviate the side effects of certain medications that treat arthritis and other autoimmune conditions.
When left untreated, arthritis can cause permanent pain. An effective treatment plan can help you keep your symptoms under control and assist you in maintaining a normal, healthy and balanced life. Many people with arthritis can maintain a fitness routine and continue working at their jobs.
For the most part, osteoarthritis cannot be prevented. Wear and tear on your joints, bones, cartilage and ligaments is a natural part of aging. Regardless, it’s possible to control osteoarthritis by making specific changes to your routine. For instance, you may notice that particular actions or motions will aggravate your condition, and you can limit these to reduce pain. But even if you’re seeking regular treatment, many other types of arthritis aren’t possible to prevent. For instance, rheumatoid arthritis can worsen regardless of treatment, and flare-ups can be challenging to control or predict.
All types of arthritis require consistent medical care. When the condition is detected and diagnosed early, the symptoms of arthritis can be treatable and suppressible. Even autoimmune forms of arthritis such as rheumatoid arthritis are more controllable when you’re managing them under a doctor’s care. If left untreated, arthritis can cause permanent damage, deformities and even organ failure, depending on the severity and type of arthritis.
Arthritis can impact your quality of life, especially if you’re younger. Talk to a medical professional about any symptoms of depression or sadness that you experience. A doctor or mental health specialist can work with you in processing and coping with these emotions to help you lead a more enjoyable life.
Resource Links:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4349405/
https://www.nature.com/subjects/osteoarthritis/nrrheum
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(19)30417-9/fulltext





