
Atopic dermatitis is an inflammatory skin condition characterized by dry, itchy skin, which often comes and goes in what’s known as a relapsing-remitting fashion. Living with atopic dermatitis can be frustrating because of the sensations this condition causes in your skin, but there are many treatment options available, even if you have severe symptoms. And just as important as finding the right treatment is learning how to minimize or prevent symptomatic flares. Here’s what you need to know about treating atopic dermatitis and finding relief.
What Is Atopic Dermatitis?
Atopic dermatitis is the most common type of eczema; the term “eczema” is often used synonymously with atopic dermatitis. It affects people of all ages and usually first presents in early childhood before the age of 5. Some children outgrow the condition entirely, but for many it reappears in adulthood. It’s usually chronic, and symptoms can come and go as flares or relapses that occur with varying frequency. Atopic dermatitis is more common in people with a family history of the condition and in those who have other atopic conditions such as allergies, hay fever (allergic rhinitis) and asthma.
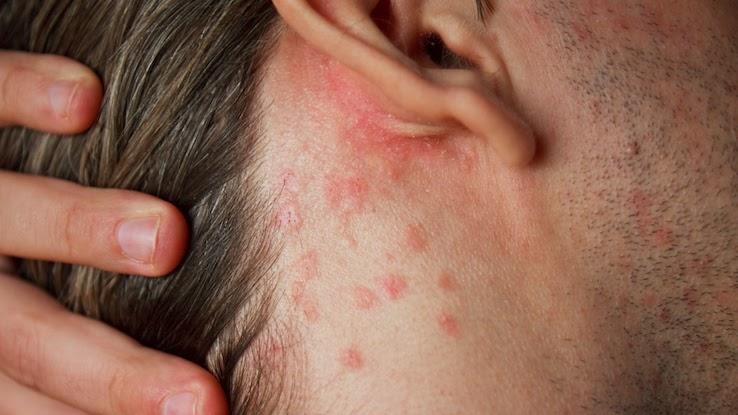
What Are the Symptoms of Atopic Dermatitis?
The hallmark symptoms include a red, itchy rash that tends to get worse at certain times, often with identifiable triggers. The rash typically affects areas known as “extensor surfaces,” which include inner elbows, the back of the knees, inner wrists and ankles. In infants, the rash also typically affects the cheeks, forehead and scalp. However, atopic dermatitis can affect any part of your skin’s surface.

Affected skin can become incredibly dry, cracked and scaly, and there might be physical damage to the skin caused by excessive scratching. Damaged skin can become infected, leading to redness, pus and sores. Over time, damaged skin can become thickened, which is known as lichenification and appears as rough white areas.
What Causes Atopic Dermatitis?
The exact cause of atopic dermatitis is a combination of genetic and environmental factors. At the root of the condition is your immune system’s inability to maintain your skin properly. It results in your skin losing its ability to maintain moisture and protect against irritants, bacteria and allergens. The environment also plays a role, with atopic dermatitis being more common in people who live in urban areas compared to those in rural areas.

Research has also shown that some people with eczema and atopic dermatitis don’t have enough filaggrin, a protein that helps form a protective barrier on the surface of the skin. Without this barrier, moisture tends to escape and can allow viruses and bacteria to enter the skin. Along with the trauma caused to an affected area by repeated scratching, this lack of moisture makes the skin especially prone to infections.
What’s the Best Way to Treat Atopic Dermatitis?
There is currently no cure for atopic dermatitis, but there are many treatments and home remedies available to help relieve symptoms. The first-line treatment option is to use topical therapies, which typically include creams and ointments you apply directly to your skin.

The most commonly recommended topical therapy is an emollient. Emollients are moisturizers you can use every day, regardless of whether you’re experiencing symptoms or not. These work to keep your skin in a healthy condition and reduce the frequency of flares.
Emollients come in many different forms, from thin lotions to thick ointments. Thin lotions are useful for areas of the skin that are hairy and for areas that are wet due to infection. Thicker creams are best for typical everyday use as they’re effective at moisturizing and your skin can quickly absorb them. Ointments are greasier and better suited to areas of particularly thickened skin. Ointments are commonly recommended for application at night to reduce any transfer to clothing and to give your skin more time to absorb them.
When your skin is actively inflamed during a flare, a topical treatment using corticosteroids is often recommended. Steroids work to limit immune system overactivity and reduce inflammation. Treatment with topical steroids is usually reserved for flares, as long-term application can cause thinning of the skin. Corticosteroids come in different forms and strengths, and treatment usually starts with the lowest strength of steroid, only increasing if one doesn’t control your symptoms.
Some cases may not respond to topical treatment options and might require additional forms of treatment. Oral corticosteroids are an option for moderate to severe cases but aren’t intended for long-term use because of the potential for serious side effects. Ultraviolet light therapy is also sometimes used in cases of atopic dermatitis that hasn’t responded to topical therapies.
New treatments are also emerging, and these include what’s called biological therapy. Biological therapy alters your body’s production of certain chemicals and can directly “turn off” those that cause inflammation in atopic dermatitis. These therapies are normally injected into your skin or administered into a vein as an infusion. They’re reserved for patients with very severe atopic dermatitis that hasn’t responded to topical or oral therapies.
You might also need to take additional medications. For example, you may need antibiotics if your skin becomes infected. Or, you might take antihistamines if your itching is particularly bothersome or disrupting your sleep.
Treating atopic dermatitis isn’t always straightforward and may require trying several methods before you find the best solution. It’s also important to remember that atopic dermatitis is characterized by periodic flares followed by remission, which means that symptoms can return at any time.
Often, people with atopic dermatitis can identify triggers that cause a flare or worsen symptoms. Common triggers include certain fabrics, excessive heat and sweating, soaps and detergents, and stress. It can be helpful to keep a diary of your symptoms to try to identify potential triggers.
Resource Links:
https://nationaleczema.org/eczema/types-of-eczema/atopic-dermatitis/
https://www.aad.org/public/diseases/eczema/types/atopic-dermatitis
https://bestpractice.bmj.com/topics/en-gb/87
https://www.nhs.uk/conditions/atopic-eczema/
https://medlineplus.gov/genetics/condition/atopic-dermatitis/





